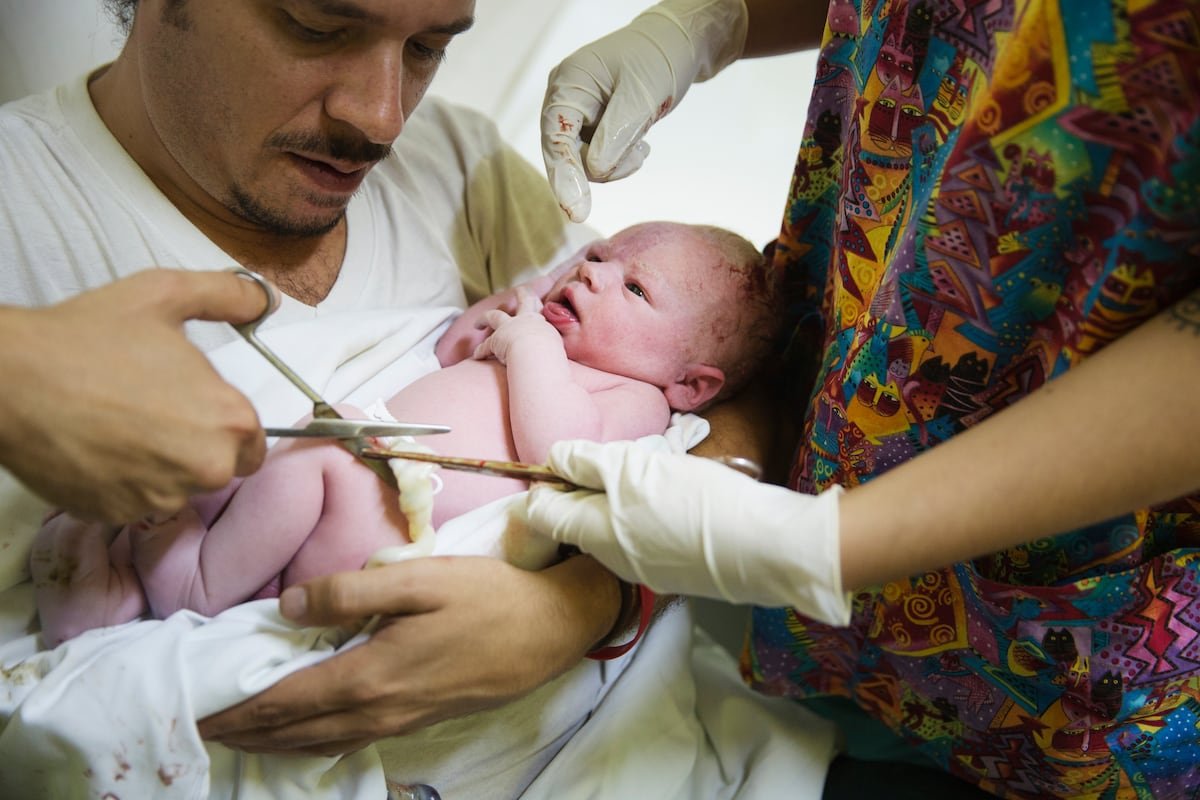
Julia’s final birthing class at her private clinic consisted of an informational session. A company representative came to talk to the future parents of the benefits linked to saving their baby’s umbilical cord blood. It could be useful, they were told, because such blood has great potential in regenerative medicine and perhaps, as science advances, its stem cells could help to cure your child or their siblings’ eventual illnesses. The presentation was based more in hypothesis than reality.
The probability that frozen tissue will benefit the person who froze it is remote. The chance of developing acute lymphoblastic leukemia, the most common childhood cancer, currently stands at one in 20,000. And frozen cells may not always be useful in treating the disease, for which other alternatives are more widely employed. Other estimates reduce the chance of its use by several orders of magnitude.
Parents are looking at a bill of $1,700 to $2,400 for preserving these samples for two decades. VidaCord, the company that gave the talk at Julia’s birthing class, is a Spanish pioneer in the field, and has yet to use any of the roughly 20,000 cords that it has frozen since it was founded more than a decade ago.
With approximately the same number of active stored samples (and having received 61,000 donations in total), the Center for Transfusion, Tissue and Cells in Málaga, Spain’s largest public cord blood bank, has carried out a thousand interventions for third‑party recipients around the world. Most have been to treat leukemia, although given the shrinking demand for its treatment, the bank’s administrators are looking for new applications for the samples, and using them for research.
The dilemma many parents face when they’re given information or read the promotional brochures often found in gynecology clinics is whether to donate cord blood altruistically so it can be used for anyone who might need it, or to store it in a private bank for family use — as a potential cure for leukemia or other conditions currently under study, though its effectiveness has not yet been demonstrated.
Ángel Álvarez, president of VidaCord, thinks the latter option is a worthwhile investment. “It’s more or less the cost of an iPhone, and though the probability it will be used is low, its possible benefit is tremendous. There are 120 ongoing investigations, some of which, like that of diabetes, are quite advanced.”
However, most voices in the world of oncohematology and medical-scientific societies disagree. Rafael Matesanz, who was director of Spain’s National Transplant Organization when private umbilical cord blood banks were approved in the country in 2006, sums up his perspective as follows: “They sell hope, like so many things in medicine.”
Matesanz is asked whether he would recommend private banks to future parents who are having doubts as to what to do with their umbilical cord?
“To any family member, friend or coworker who asks me this, I tell them, no way,” he answers. “I’ve had two grandkids and of course, it didn’t occur to me to tell [their parents] to save their cells. It doesn’t make sense. Before [when private banks were made legal] we said they weren’t going to work. Now, we see they haven’t worked.”
In between these two perspectives, one finds that of José María Moraleda, a professor emeritus of hematopoietic transplants and cell therapy at the University of Murcia. He researches possible future applications of the cells in umbilical cord blood and insists several times that this makes him “biased.”
Moraleda concedes that nowadays, freezing blood for one’s family is of almost no use, even though there have been very concrete, isolated cases in which it has been used. But he believes that the cells this blood contains are full of the potential to cure illnesses in the future. “There are already signs that they can improve parameters in some children with autism, paralysis, metabolic diseases that cannot otherwise be treated. There is hope,” he says.
When asked would he recommend the process to future parents, he replies: “I think that in the future, umbilical cord blood is going to work. I would recommend that they save it in a public bank. But other people may use it if it’s there. If they want to preserve it for themselves and they’re able to do so, I wouldn’t tell them not to,” says Moraleda.
Potential of cells
The potential of these cells lies in their immaturity, which means they can be manipulated to form part of the tissue of other organs. For example, there have been experiments in repairing cardiac damage that have gone well, though there is a long path ahead for such studies to be translated into everyday treatment, if they ever are. Possible applications in neurodegenerative diseases like Parkinson’s are also being investigated.
In the field of hematology, their potential utility in treating leukemias and other blood diseases is linked to the fact that they contain stem cells capable of regenerating bone marrow that has been damaged by chemotherapy or the disease itself. Since its cells are younger, and less reactive than those of an adult donor, the risk of rejection is reduced, and transplants can be carried out without complete compatibility, which is particularly valuable for patients who do not have a totally adequate donor on hand.
Their use in babies themselves, however, has clear limitations. If the child develops hematological cancer in the future, like leukemia, it’s likely that their umbilical cord blood carries the predisposition of developing the tumor. That means it would not be advisable to use it in treatment.
For third-party recipients, the use of these cells has also declined, largely because there are now other sources of stem cells for bone marrow transplantation. Though a certain degree of compatibility is still necessary, haploidentical transplantation — in which half of the genetic markers match — has become a practical and accessible option. As Luis Felipe Casado, head of the hematology department at HM Madrid hospitals, explains, almost all patients have at least one first-degree relative, such as a parent, sibling or child, who can act as a donor.
Current uses
Umbilical cord blood is still useful, explains Laura Ponce, medical director of the Center for Transfusion in Málaga, in urgent transplants, for cases in which no compatible marrow donors can be located. “They are products that have undergone quality testing and are ready to use,” she says.
At the public bank where she works, cells are also turned into eye drops that are useful for certain eye conditions for which other medications have failed as treatment. When asked what she would recommend to future parents, Gracia García, director of the Málaga center, advocates for “solidarity and altruism,” though she is loathe to enter into conflict with private banks. “What I do recommend is that if someone wants to store their child’s cord, they should make sure they do so with a certified company that offers every guarantee,” she emphasizes.
Sergi Querol, director of the Bone Marrow Donor Registry, says: “At the moment [freezing with a private bank] doesn’t do anything and the probability [that will change] is one in a million. If your child develops leukemia, they will not be treated with those cells. If [parents] think that it is beneficial, they’ll do it, but at the moment, it is not something that is worth anything.”
Most of these centers offer to store the blood abroad, since Spanish law requires that if the samples remain within national territory, their tissue data must be registered in the Bone Marrow Donor Registry (REDMO) and made available for use by other people if needed. Only 1% of the families who have stored their children’s tissues with VidaCord have chosen to keep them in Spain.
Ultimately, Julia decided not to preserve her daughter’s tissue, despite receiving two calls from the company trying to convince her otherwise. Diego and Irene (all parents’ names in this article are aliases) did decide to preserve their children’s. They were also spoken to about freezing the blood in a birthing class.
“They created a sense of need for us,” Diego says. He is a carrier of a genetic disease that is recessive, in principle — but the risk involved made them decide to go with a private bank. Diego explains that, “In the end, we decided the financial cost was relatively affordable and that it might be useful in the future, considering that I have this disease. We are aware that it will probably not work, but we are looking for hope in the face of a hypothetical problem, for the ‘what if’ scenario.”
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition